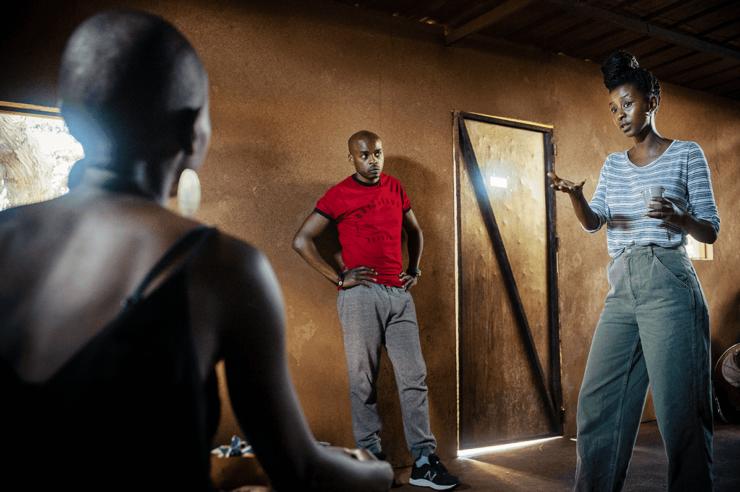Around the world, 200m women alive today have undergone female genital mutilation. Now a grassroots project is piloting an approach that helps to heal the mental scars that mean the practice is passed down through generations
Zeitun Abas is still haunted by the memory of her circumcision at the hands of her grandmother, and the three other women who held her down. “I remember the sight of blood-stained sacks spread on the hut floor and a razor blade. [The memory] makes me scared all over again.”
The Kenya-based Somali mother of three was subjected to female genital mutilation (FGM) aged six, and now at 29, she admits to repeatedly contemplating suicide.
Abas is not alone. Some 16 per cent of Kenyan women and girls are subjected to FGM; worldwide, it’s estimated that 200m women alive today have been cut. The effects on mental health are considerable, from anxiety to PTSD, and yet the discourse around ending the practice has always focused on the physical rather than mental impacts of FGM.
Last year, however, a Kenyan NGO launched a programme with a radically different approach – intergenerational healing and trauma-informed support for the women who have survived FGM. This small project has lofty aims – to finally break the cycle and bring an end to a practice they believe should be called, plain and simply, “sexual assault”.
Based in Nairobi, The Girl Generation (TGG) is an ambitious five-year, UK government-funded project exploring ways to bring an end to FGM. Addressing emotional trauma was the starting point of their new programme, the Survivor Leadership Training (SLT), which first piloted last March for 20 Kenyan women.
Designed by the Somali-born, British FGM survivor and psychotherapist Leyla Hussein – the project’s global advocacy director – she wanted it to be “girl-centred”. Until now, says Hussein, FGM activism was “colonised by men – always a conversation with community or religious leaders. No one was listening to the survivors.”

Some survivor-leaders use art to confront FGM. Image: Khadija Farah
Key to TGG’s approach is to push for recognition of FGM as sexual violence and a human-rights violation, rather than a cultural tradition. “Language is key,” says Hussein. “Putting a sharp object to a child’s genitalia is an act of sexual assault.” To this end, the course provides psychosexual health education, including reproductive health and rights, reframing the practice in the minds of survivors.
Abas took part in the programme three months ago, where mothers and daughters are encouraged to share their stories in a safe space. Here, finally, the possibility of healing the mother-daughter relationship – so often damaged by FGM – is enabled. For many, it’s the first time such matters are discussed – daughters gain some understanding of why their mothers inflicted the practice upon them, while mothers get to share their own pain.
The practice is so culturally entrenched that it has proven hard to end. Especially in rural communities, uncut girls are considered dirty and unmarriageable, which means they are more at risk of sexual violence and may also miss out on a much-needed dowry. Cutting is usually performed without anaesthetic by “the people most connected to them”, explains Ann Njuguna, communications manager of TGG. “[Being cut by family members] makes you lose trust with people,” she explains, “and you grow with anger, shame and uncertainty, which affects self-esteem. Some survivors don’t even have the self-esteem to pursue an education.”
Women are saying, ‘we will never subject our daughters to this pain. It has to end with us’
Amongst FGM survivors, mental health issues such as anxiety, anger, depression, PTSD, alcohol and drug abuse, sexual dysfunction and relationship breakdowns are prevalent, Njuguna reports. The issue is worsened by the fact that mental health is barely recognised in rural areas: “Nobody wants to talk about it or cares what you’re going through,” she says. And because FGM is a traditional practice, she adds, “It’s [considered] OK to be in a lot of pain.”
As well as excruciating menstrual pain, Abas suffered nightmares and insomnia, and because of extreme pain in childbirth, vowed not to have more children, going against the Somali culture of having large families as a sign of prestige. All this culminated in a sense of despair for the young mother.
Despite her initial shyness, Abas gradually found her voice: “Through the programme, I realised many survivors underwent more painful experiences than me. I realised there was a need to accept what had happened and move on. Being able to confidently engage in conversations around FGM, I no longer feel as bitter.”

Hafsa Dida and her mother, Hawa Dida, who attended a mother-daughter forum together to speak about their experiences with FGM. Image: Khadija Farah
Having found the confidence to set up her own small business selling soap and detergent in Isiolo Town, earning enough to support her family, she says that she will never subject her daughters to the same experience she went through at the hands of her loved ones.
The programme also nurtures survivors’ leadership skills, so that they can start their own support groups and help other women. Several survivor-leaders have started mother-daughter forums; others use art and photography as vehicles to discuss FGM. Meanwhile, two trainees have become leaders in county government: “Many [politicians] are afraid to speak out because they’re afraid of losing votes,” says Njuguna, “but after the training [these women] were more confident talking about FGM.”
Although this “train the trainer” model is initially expensive – costing about $1,000 (£780) per participant – it can be a cost-effective solution to addressing both the mental health impact of FGM and bringing the practice to an end, because survivor-leaders “cascade” their training to their communities. TGG offers grants so leaders can, for example, hire a psychotherapist to provide support for survivors, or pay for an event space or materials; the grants range from $2,000-$3,000 (£1,570-£2,350) per person.

Zeitun Abas Omar (center) discusses her experience of FGM at a meeting in Isiolo. Image: Khadija Farah
Although the data remains incomplete, TGG estimates that the first cohort has reached about 300 additional women and girls. They are already witnessing a rupture of the FGM cycle: “Women are saying, ‘we will never subject our daughters to this pain. It has to end with us.’” says Njuguna. “We are also seeing many more people discussing FGM – it’s becoming less taboo.”
TGG also claims that the mental health of SLT participants has improved, as evident in their qualitative data. “After SLT, most are able to confidently say they realise what has happened to them, and are able to stop blaming themselves,” says Esmael Omar, TGG’s head of policy and advocacy. “Also, most were able to name their feelings, channel their anger in a healthy manner, and manage their emotions with learnt self-care skills.”
Being able to confidently engage in conversations around FGM, I no longer feel as bitter
Dr Abubakar Hussein, director of health of Kenya’s Isiolo county, said the mother-daughter initiative “has gone a long way in helping take care of the mental health of survivors”.
However, TGG accepts that its research is limited. “We need more qualitative data to help us understand things better,” says Omar. Also limiting is the lack of funds. “There are more people in need than we can cater for,” says Njuguna. “We are currently focusing on three counties in Kenya, but FGM is practised in more than 20 out of 47.”
With only one trained cohort so far, it’s early days for SLT. “We’re now looking at cascading the curriculum this July to a regional level in Kenya, and also to Somaliland, Ethiopia and Senegal,” says Njuguna. TGG says that it will continue documenting what works and what doesn’t in order to develop guidance notes – the longer-term plan is that there will be an online curriculum, as well as an Africa-wide network of survivor-leaders raising awareness. The ultimate aim, says Omar, is that “anybody will be able to access the tools, and we can finally end the cycle of FGM”.
Images: Khadija Farah
 Developing mental wealth is a series produced by Positive News and funded by the European Journalism Centre, through the Solutions Journalism Accelerator. This fund is supported by the Bill & Melinda Gates Foundation
Developing mental wealth is a series produced by Positive News and funded by the European Journalism Centre, through the Solutions Journalism Accelerator. This fund is supported by the Bill & Melinda Gates Foundation
Help us break the bad news bias
Positive News is helping more people than ever to get a balanced and uplifting view of the world. While doom and gloom dominates other news outlets, our solutions journalism exists to support your wellbeing and empower you to make a difference towards a better future. And as Positive News’ audience and impact grows, we’re showing the rest of the media that good news matters.
But our reporting has a cost and, as an independent, not-for-profit media organisation, we rely on the financial backing of our readers. If you value what we do and can afford to, please consider making a one-off or regular contribution as a Positive News supporter. Give once from just £1, or join 1,000+ others who contribute an average of £3 or more per month. You’ll be directly funding the production and sharing of our stories – helping our solutions journalism to benefit many more people.
Join our community today, and together, we’ll change the news for good.